
Breast cancer remains a significant health concern for women throughout the globe. In Singapore, it stands as the most common type of cancer among women. The Singapore Cancer Registry [1] reported that breast cancer accounts for nearly one in three cancer diagnoses among women in the country. This translates to 29.7% [2] of all female cancers, with approximately 1,100 new cases diagnosed annually. However, what is even more concerning is the fact that roughly 270 women [3] succumb to the disease each year.
Due to its prevalence, early detection through regular screening plays a critical role in improving the survival rate. In fact, research shows that early diagnosis can increase the chances of successful treatment by as much as 90% [4].
The aim of breast cancer screening is to identify the cancer at its earliest stage, ideally before symptoms are noticeable. By detecting cancer early, women have more treatment options available and a greater likelihood of successful outcomes. This guide will provide a comprehensive overview of the breast cancer screening options available today, from blood tests to mammograms and how each method can contribute to early detection.

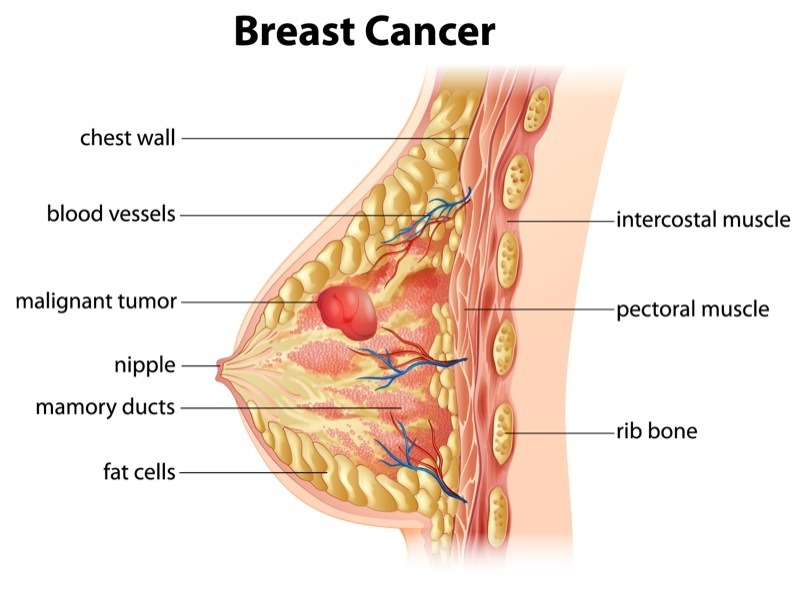
Breast cancer screening refers to the preventive measures taken to detect breast cancer before any symptoms emerge. Unlike diagnostic tests that are performed when there are visible signs or symptoms of breast cancer, screening is done on seemingly healthy individuals, especially among those with a family history of breast cancer. The primary objective of screening is to identify cancer early, ideally when it is confined to the breast tissue, and has not spread to other parts of the body.
Regular breast cancer screening is essential for all women, particularly those over the age of 40 years old or those with a family history of breast cancer. However, women with other high-risk factors as listed below may need to begin screening early:

It is important to understand that consistent screening can significantly improve a woman’s chance of beating the cancer, as early detection may also include the following benefits:
Be that as it may, it is crucial to choose the appropriate screening method based on individual risk factors, age, and lifestyle. In fact, working closely with a licensed and qualified medical practitioner will be advantageous, as they can help tailor a screening plan that best suits each woman’s needs.
There are various screening methods available today, each with its own unique benefits and limitations. These include blood tests, imaging techniques like mammograms, ultrasounds, and magnetic resonance imaging (MRI) for those at high risk. While there are many options available, the choice of screening method often depends on the individual’s risk profile and medical history. The following briefly describes each method:
Each method plays a different role in breast cancer detection, and often, a combination of these tests may be necessary for comprehensive screening.
Blood tests are often used to detect early signs of breast cancer. These tests work by identifying specific proteins or markers that cancer cells release into the bloodstream. To give an example, markers like CA 15-3 and CEA can sometimes indicate the presence of cancer, although these markers are not exclusively specific to breast cancer.
Even so, blood tests are valued for their non-invasive nature. They can be conducted quickly, with results available in a shorter time frame compared to imaging techniques. However, while blood tests can provide valuable information, they are not typically used as standalone diagnostic tools. Their sensitivity and specificity are limited, meaning that they are better suited as supplementary tests rather than primary screening tools.
That being said, blood tests are particularly useful for monitoring patients who have already been diagnosed with cancer to track the effectiveness of treatment or detect recurrences. Be that as it may, as a screening tool, blood tests should be paired with other methods like imaging for a more accurate diagnosis.
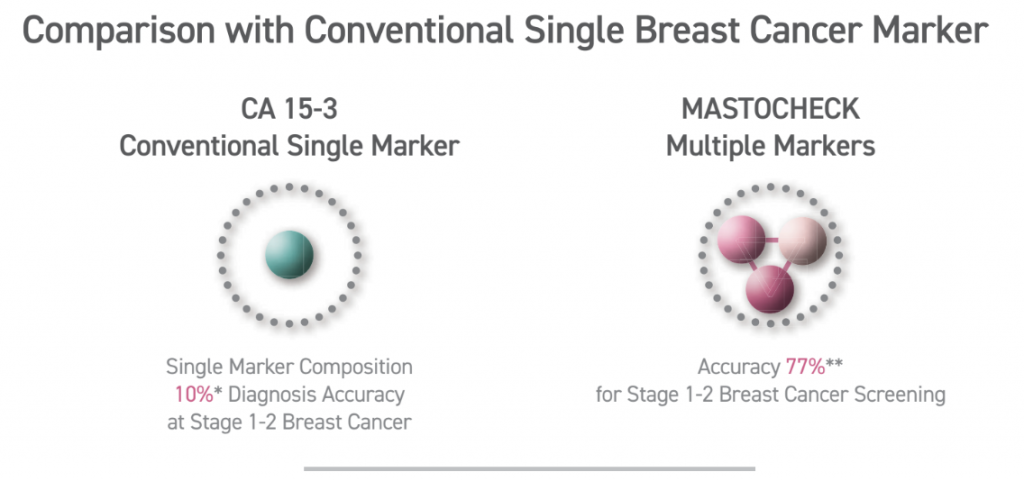
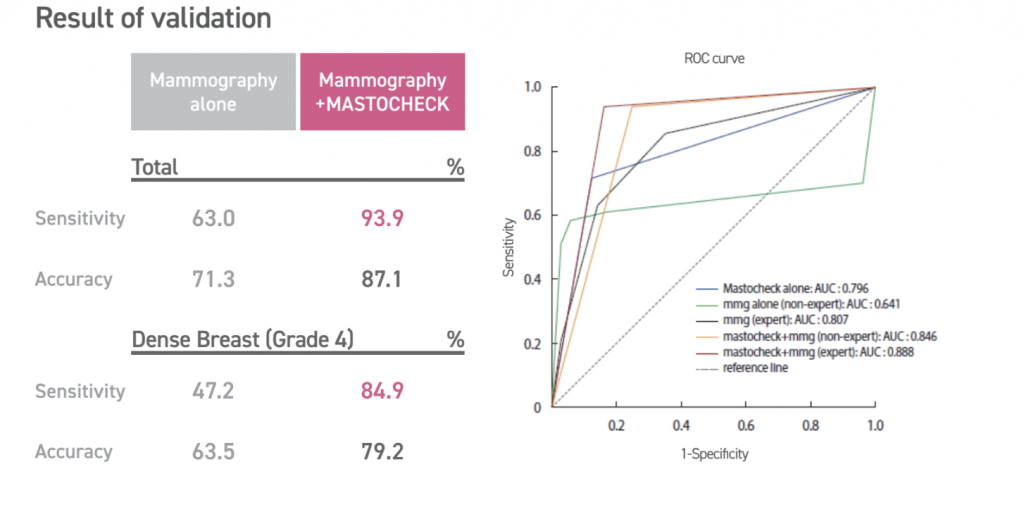
Unlike traditional blood tests that focus solely on inherited mutations, Mastocheck utilises advanced proteomic analysis to identify tumour-related proteins which are released by cancer cells and can serve as early indicators of tumour presence. This test is non-invasive, requiring only a blood sample, and can identify cancerous changes (disease-specific expression patterns) before they become visible through imaging. Hence, proteomics-based early diagnosis technology, like Mastocheck, greatly maximises diagnostic accuracy — with about 77% accuracy for stage 1-2 breast cancer.
However, it is essential to understand that while various blood tests can provide valuable insights into cancer risk, it is not a replacement for imaging techniques. Rather, it serves as a complementary tool, especially for those at higher risk of cancer (shows 10%-30% higher sensitivity compared to Mammography alone). Knowing your current cancer status through Mastocheck can help navigate the decision-making process regarding the frequency of follow-up screenings or the need for further diagnostic imaging.
The benefits of Mastocheck screening include:
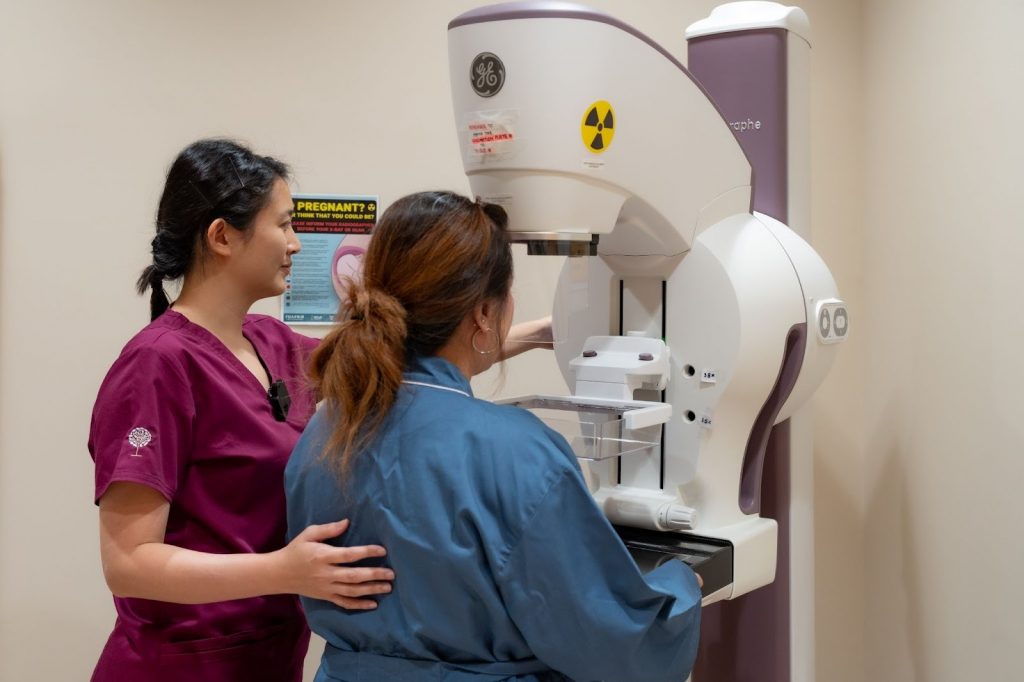
Mammograms remain one of the most reliable screening tools for early breast cancer detection. This method involves using low-dose X-rays to examine breast tissue for any signs of tumours or abnormal growths [17]. For women aged 40 and above, regular mammograms are often recommended, as the risk of developing breast cancer increases with age.
A screening mammogram is typically done once every one to two years for women at average risk, while those at higher risk may need to undergo mammograms more frequently.
The benefits of mammograms are well-documented. In fact, they have been shown to reduce breast cancer mortality by enabling earlier diagnosis. However, some women may find the procedure uncomfortable due to the compression of breast tissue required for clear imaging. Additionally, mammograms do expose women to a small amount of radiation, but the risk is generally outweighed by the benefits of early detection.

While mammograms are effective for most women, certain cases may require additional imaging techniques, like ultrasounds, and MRIs.
Ultrasound imaging is particularly useful for women with dense breast tissue, where mammograms may not be as effective [18]. Dense tissue can obscure tumours, making them harder to detect. Ultrasound also works using sound waves to create images of the breast tissues, allowing for better visualisation of abnormalities that may not appear on a mammogram.
Meanwhile, MRI is an advanced imaging technique, typically for high-risk individuals. MRIs use magnetic fields, and radio waves to create detailed images of the breast, making it possible to detect cancers that might be missed by mammograms, or ultrasounds. In fact, women with a strong family history of breast cancer, or those with known genetic mutations like BRCA1, or BRCA2 may benefit from regular MRIs in addition to mammograms.
Both ultrasounds and MRIs serve as complementary tools to mammograms, and are usually recommended when additional clarity is needed.
Early detection of breast cancer greatly improves survival rates and treatment outcomes. In fact, there is a 5-year relative survival rate for localised (tumour is confined to breast tissue) breast cancer is approximately 99%. This makes early detection of breast cancer and timely treatment paramount.
Combining a Mammogram with Mastocheck allows your doctor to detect structural changes in breast tissue and molecular changes in biomarkers that indicate early-stage breast cancer, offering a comprehensive significantly reducing the chances of false negatives.
Undergoing a Mastocheck blood test can also reduce your need for unnecessary procedures and additional stress. This is because it provides additional confirmation when ambiguous findings are detected via the mammogram, helping differentiate between the benign and malignant abnormalities in the breast.
Breast cancer screening can feel overwhelming, especially when you are unsure what to expect. Our doctor provides careful guidance throughout the process to help you feel informed and reassured. Below is a step-by-step overview of the general breast cancer screening procedures offered at our clinic.
Breast cancer screening typically begins with an initial consultation with a doctor. During this appointment, your medical history will be reviewed, including any personal or family history of breast cancer. The doctor may also ask about your lifestyle, current symptoms and other risk factors that could influence your screening plan. This assessment helps determine the most appropriate screening approach based on your individual risk profile.
If a blood test such as Mastocheck is included in the screening plan, the procedure is usually quick and straightforward. A small blood sample is drawn from a vein in the arm and sent to a laboratory for analysis to detect potential cancer markers. The process typically takes only a few minutes and involves minimal discomfort, similar to a routine blood test. Most individuals can resume their normal activities immediately afterwards, while results are usually available within a few days to a week.
If a mammogram is recommended as part of the screening process, you may be asked to change into a gown and remove any jewellery or clothing above the waist. During the procedure, the breast is positioned on a flat surface and gently compressed with a clear plastic plate to obtain clear images of the breast tissue. The compression may feel slightly uncomfortable, but it lasts only a few seconds.
Images are taken from different angles, usually two views per breast, and the entire procedure typically takes about 20 minutes. After the imaging is completed, the images are reviewed for any signs of abnormalities. Results are usually available within a few days. If any suspicious findings are detected, additional diagnostic tests or imaging may be recommended.
An ultrasound may be recommended for women with dense breast tissue or when additional imaging is required. During the procedure, you will lie comfortably while a gel is applied to the breast area. A handheld device called a transducer is then moved over the skin to create images of the breast tissue using sound waves. The examination is painless and usually takes about 15 to 30 minutes.
After the screening tests are completed, a follow-up consultation may be arranged to review and discuss the results. If any abnormalities are detected, the doctor will explain the findings and advise on the next steps. These may include further imaging tests, additional evaluations, or a biopsy to determine whether cancer is present.

Being well-prepared can help ensure a smooth and effective screening experience. To help you prepare for your breast screening, here is a detailed guideline to get you started.
When scheduling an appointment for breast screening, do remember to pick a date at least a week after your menstrual period. This is due to the fact that your breasts are less likely to be tender during this time. Doing so can help minimise discomfort during the procedure. Additionally, for women undergoing blood tests or other non-imaging tests, there are no specific timing requirements.
On the day of your screening, wear a two-piece outfit so that you can easily remove your top piece of clothing for imaging procedures. Avoid wearing deodorant, antiperspirant, powders or lotions on your underarms or breasts, as these products can show up on mammogram images as white spots, potentially leading to false alarms.
It is important to bring your identification, health insurance information, and any prior imaging results if you have been screened before. Having these past records allows our doctors and radiologists to compare images and detect any subtle changes in breast tissue over time.
If you are concerned about discomfort during a mammogram, consider taking an over-the-counter pain reliever, such as ibuprofen or acetaminophen, about an hour before your appointment. This can help alleviate any pain associated with breast compression. However, always speak with your doctor before taking any medication to prevent any complications.
If you are scheduled for an MRI, inform the technician if you have any metal implants, pacemakers, or allergies, particularly to contrast dyes. You may need to fast for a few hours before the test if a contrast dye is being used. Additionally, do remember to remove any metal objects, such as jewellery, belts or watches, before the scan, as this can disrupt the imaging process.
For some women, the thought of undergoing a breast cancer screening can be anxiety-inducing, especially if it is their first time. But do remind yourself that these screenings are proactive steps toward maintaining your health, rather than dwelling on the possibility of malignancy. Some tips that can help ease your nerves before your appointment include deep breathing exercises, or listening to calming music. In fact, if asking questions can help reduce your anxiety, then do feel free to speak with our doctors to help you be more mentally prepared for the screening.
After your screening, there are generally no restrictions and you can resume your normal activities immediately. However, if you experience any soreness after a mammogram, applying a cold compress can help reduce discomfort. For blood tests, keep the bandage on for a few hours to avoid bruises.
By following these preparation steps and understanding what to expect, you can make your breast cancer screening experience as comfortable, and stress-free as possible.

| Feature | Mammogram | Ultrasound | MRI | Mastocheck |
| Purpose | Standard screening for breast cancer. | Complements mammograms and can be used to evaluate dense breast tissue. | High-sensitivity breast cancer screening for high-risk patients. | Blood test for early detection of specific biomarkers for breast cancer. |
| Recommended for | Women over the age of 40 years old or have risk factors for breast cancer. | Women with dense breasts, palpable lumps or other possible breast cancer indicators. | High-risk individuals. | Early detection or supplemental screening. |
| Technology | X-ray imaging, may sometimes include a contrast for Contrast Enhanced Mammogram (CEM). | Utilises targeted ultrasound waves to visualise breast tissue structures. | Utilises magnetic fields and contrast dye to visualise breast tissue structures. | Blood sample analysed for cancer markers. |
| Sensitivity | High sensitivity, but may not be as effective for dense breast tissue | High sensitivity, but may miss small or early cancers. | Very high sensitivity, detects small, early-stage cancers. | High sensitivity and provides risk indication for early cancers, but not the specific tumour location. Good early-warning tool. |
| Radiation exposure | Low-dose radiation. | None. | None. | None. |
Breast cancer screening plays an important role in detecting cancer early, often before symptoms appear. Choosing the most suitable screening approach depends on several personal factors, including age, family history, genetic risk, and overall health. Understanding the available screening options allows you to make informed decisions and take proactive steps to safeguard your well-being.
For many women in their 40s, annual mammograms are commonly recommended. Women with higher risk factors or specific clinical indications may benefit from additional screening methods, such as Mastocheck testing or breast ultrasound. A consultation with an experienced doctor is important to determine the most appropriate screening strategy based on your individual risk profile. A personalised plan helps optimise early detection while providing reassurance that your breast health is being carefully monitored.
If you are considering breast cancer screening or would like guidance on the most suitable options for you, arrange a consultation (link to ‘Contact Us’ page) with our doctor. A professional assessment can help determine the right screening approach and support you in taking confident, proactive steps toward protecting your breast health.
References
[1] Breast Cancer. (n.d.). In www.singaporecancersociety.org.sg. Retrieved November 14, 2024, from https://www.singaporecancersociety.org.sg/learn-about-cancer/types-of-cancer/breast-cancer.html
[2] [3] Jara-Lazaro, A. R., Thilagaratnam, S., & Tan, P. H. (2010). Breast cancer in Singapore: some perspectives. In Breast cancer (Tokyo, Japan) (Vol. 17, Issue 1, pp. 23–28). Breast cancer (Tokyo, Japan). https://doi.org/10.1007/s12282-009-0155-3
[4] By. (n.d.). The landscape of breast cancer screening and treatment in Singapore. In how well do we know it. Retrieved November 14, 2024, from https://www.singhealth.com.sg/news/medical-news-singhealth/landscape-breast-cancer-screening-treatment-singapore
[5] CDC. (2024). Breast Cancer Risk Factors. In Breast Cancer. https://www.cdc.gov/breast-cancer/risk-factors/index.html
[6] Dense Breasts: Answers to Commonly Asked Questions - NCI. (2018). In www.cancer.gov. https://www.cancer.gov/types/breast/breast-changes/dense-breasts
[7] Diethylstilbestrol (DES) Exposure and Cancer - NCI. (2021). In www.cancer.gov. https://www.cancer.gov/about-cancer/causes-prevention/risk/hormones/des-fact-sheet
[8] Brewer, H. R., Jones, M. E., Schoemaker, M. J., Ashworth, A., & Swerdlow, A. J. (2017). Family history and risk of breast cancer: an analysis accounting for family structure. In Breast cancer research and treatment (Vol. 165, Issue 1, pp. 193–200). Breast cancer research and treatment. https://doi.org/10.1007/s10549-017-4325-2
[9] Petrucelli N, Daly MB, Pal T. BRCA1- and BRCA2-Associated Hereditary Breast and Ovarian Cancer. 1998 Sep 4 [Updated 2023 Sep 21]. In: Adam MP, Feldman J, Mirzaa GM, et al., editors. GeneReviews® [Internet]. Seattle (WA): University of Washington, Seattle; 1993-2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK1247/
[10] Breast cancer and hormone replacement therapy: collaborative reanalysis of data from 51 epidemiological studies of 52,705 women with breast cancer and 108,411 women without breast cancer. Collaborative Group on Hormonal Factors in Breast Cancer. (1997). Lancet (London, England), 350(9084), 1047–1059.
[11] Eaton L. (2002). Early periods and late childbearing increase risk of breast cancer, study confirms. BMJ : British Medical Journal, 324(7334), 386.
[12] Zeinomar, N., Phillips, K. A., Daly, M. B., Milne, R. L., Dite, G. S., MacInnis, R. J., Liao, Y., Kehm, R. D., Knight, J. A., Southey, M. C., Chung, W. K., Giles, G. G., McLachlan, S. A., Friedlander, M. L., Weideman, P. C., Glendon, G., Nesci, S., kConFab Investigators, Andrulis, I. L., Buys, S. S., … Terry, M. B. (2019). Benign breast disease increases breast cancer risk independent of underlying familial risk profile: Findings from a Prospective Family Study Cohort. International journal of cancer, 145(2), 370–379. https://doi.org/10.1002/ijc.32112
[13] Joshi, S. C., Khan, F. A., Pant, I., & Shukla, A. (2007). Role of radiotherapy in early breast cancer: an overview. International journal of health sciences, 1(2), 259–264.
[14] Liu, Y., Nguyen, N., & Colditz, G. A. (2015). Links between alcohol consumption and breast cancer: a look at the evidence. Women's health (London, England), 11(1), 65–77. https://doi.org/10.2217/whe.14.62
[15] Dehesh, T., Fadaghi, S., Seyedi, M., Abolhadi, E., Ilaghi, M., Shams, P., Ajam, F., Mosleh-Shirazi, M. A., & Dehesh, P. (2023). The relation between obesity and breast cancer risk in women by considering menstruation status and geographical variations: a systematic review and meta-analysis. BMC women's health, 23(1), 392. https://doi.org/10.1186/s12905-023-02543-5
[16] Kim, Y., Kim, H.-K., Lim, C., Kim, S., Ahn, K.-G., & Noh, D.-Y. (2022). The usefulness of a three-protein signature blood assay (Mastocheck®) for follow-up after breast cancer surgery. Journal of Cancer Research and Clinical Oncology, 149(9), 5733–5741. https://doi.org/10.1007/s00432-022-04550-9
[17] CDC. (2025, February 6). Screening for breast cancer. Breast Cancer. https://www.cdc.gov/breast-cancer/screening/index.html
[18] Madjar, H. (2010). Role of breast ultrasound for the detection and differentiation of breast lesions. Breast Care, 5(2), 109–114. https://doi.org/10.1159/000297775



9:00am to 8:30pm

9:00 am - 4:30 pm, 6.00 pm - 8:30 pm
9:00 am - 1:30 pm
2:00 pm - 8:30 pm

60 Paya Lebar Road, #02-09 Paya Lebar Square, Singapore 409051
9:00 am - 12:30 pm
2:00 pm - 5:00 pm
9:00 am - 12:30 pm

275 Thomson Road,
#01-05 Novena Regency,
Singapore 307645
9:00 am - 2:30 pm
6:00 pm - 8:30 pm (Mon, Tue, Wed & Fri)
9:00 am - 1:30 pm
2:00 pm - 8:30 pm

The Venue Shoppes,
2 Tai Thong Crescent, #01-16,
Singapore 347836
9:00 am - 3:00 pm
6:00 pm - 9:00 pm (Mon, Wed & Thu)
9:00 am - 2:00 pm
Closed

244M Upper Thomson Rd, Thomson Garden Estate, Singapore 574369
9:00 am - 3:00 pm
6:00 pm - 9:00 pm (Mon & Wed)
9:00 am - 2:00 pm

9:00 am - 4:00 pm
6:00 pm - 9:00 pm
9:00 am - 2:00 pm
Closed